Get Healthy, Stay Healthy
Pharmaceutical companies contract us to manufacture biopharmaceuticals: therapeutic proteins, vaccines and live microbial products.
Active Ingredients
Producing Vaccines by the Second
A lot of pieces need to fall into place on the journey from a vaccine to a global victory over the coronavirus pandemic. One of those pieces is Wacker Biotech. As a contract manufacturer, the company produces drug substances for pharmaceutical companies, and will also soon be making an active ingredient that will form part of a vaccine candidate for the SARS-CoV-2 coronavirus.
When Alexander Fleming discovered penicillin nearly 100 years ago, he felt that he was on the cusp of a major breakthrough. And it turned out he was right, as antibiotics have since saved millions of lives. Of course, putting Fleming’s discovery to therapeutic use took more than a decade. The production process and manufacturing capacity held up implementation, forfeiting valuable time.
As the history of penicillin shows, the struggle against bacteria and viruses plays out in more than just test tubes. From the development of a drug substance to production and distribution – diseases are conquered only when a considerable number of pieces fall into place.
“We’re incredibly proud that we can play a role in the fight against the pandemic.”
Sandra Verhaagh, Production Head at Wacker Biotech
Over the past months, an entire army of scientists has once again found itself on the cusp of a major breakthrough, with the search for a vaccine for SARS-CoV-2 shifting into high gear. The search was a success. We now have multiple vaccines that have been proven effective, and instead of taking eight to ten years, the vaccine development phase was cut to just twelve months.
The next step is production. We will need billions of doses to rein in the pandemic, and the race for available production capacity is well underway. A few candidates have been in production for months in anticipation of official authorization. But if they aren’t approved, that work will have been in vain. Pharmaceutical companies, researchers and governments throughout the world are working hand in hand to make these endeavors a success.
Wacker Biotech has more than 20 years of experience in manufacturing vaccines.

Production facilities in Amsterdam cover several floors.
Twenty Years of Experience Producing Vaccines
One of the pieces of the vaccine puzzle is Wacker Biotech. For 20 years now, this subsidiary of Wacker Chemie AG has been working behind the scenes to produce vaccines. The experts at Biotech develop production processes on a laboratory scale, while their plants produce drug substances that subsequently form part of vaccines and other innovative biopharmaceuticals. Their customers operate in the pharmaceutical and biotech industries.
One of them is CureVac, a Tübingen-based biotech company that has contracted Wacker Biotech to produce the drug substance for its Covid-19 vaccine candidate CVnCoV. Production is set to begin at Wacker Biotech’s Amsterdam site in the first half of 2021, and preparations are already underway.
The brick building housing Wacker Biotech is located in the Zuid Oost district of Amsterdam. A transparent, glass dome in the middle of the building lets in daylight. It is lined with reactors, stainless-steel tanks and computer monitors. In recent months, production has been set up here especially for manufacturing what are known as mRNA vaccines – a new class of vaccine that has raised tremendous hopes in the fight against the coronavirus pandemic. If approval is granted, there are plans to produce more than 100 million doses of CureVac’s mRNA drug substance per year at Wacker Biotech. That’s three doses of vaccine per second.
“We’re incredibly proud that we can play a role in the fight against the pandemic,” says Sandra Verhaagh, who heads up production at Wacker Biotech. It normally takes several months to transfer the production process for a customer’s vaccine so that initial test runs can begin at Wacker Biotech. But CVnCoV is following a very different timeline. “You might say we transferred the process at light speed,” she observes. The company procured special equipment for the production process, purchased raw materials and established analytical and documentation processes – a major feat for everyone involved.
Wacker Biotech
As a CDMO (contract development and manufacturing organization), Wacker Biotech pools the WACKER Group’s biopharmaceutical activities. The company works on behalf of pharmaceutical and biotech firms to make therapeutic proteins, live microbial products (LMPs) and vaccines based on microbial systems. Its portfolio extends from strain/process development and analytical testing through to production for clinical and commercial applications in compliance with good manufacturing practice (GMP) guidelines. Wacker Biotech maintains three production sites: Jena and Halle in Germany (Wacker Biotech GmbH) as well as Amsterdam in the Netherlands (Wacker Biotech B.V.).
A Broad Vaccine Portfolio
mRNA vaccines are new territory for Wacker Biotech too. Up to now, the company’s portfolio comprised conventional live and killed vaccines as well as protein-based, polysaccharide and conjugate vaccines, such as those that combat cholera or meningitis A.
“It fascinates me that we can make something that doesn’t just heal people – it is a preventive measure that keeps them healthy too,” says Verhaagh, a molecular biologist who has spent nearly her entire career working on vaccines in all of their forms. “Not all vaccines are created equal,” she explains. “One option is to use the pathogen itself as a vaccine – in either a weakened or inactive form.” The organisms in live vaccines are capable of reproducing, but they can no longer cause illness. Many of these vaccines – those that prevent childhood diseases such as mumps, measles and rubella – confer life-long immunity. Inactivated vaccines on the other hand, which are also referred to as killed vaccines, contain either a dead pathogen or part of an inactive virus to which the immune system responds. The protective immunity provided by killed vaccines generally only lasts for a few years, after which it will need to be refreshed.
Most of today’s vaccines are killed varieties developed from only select molecules of a pathogen, and these are commonly genetically engineered. These kinds of vaccines contain individual characteristic proteins of a pathogen that are intended to produce an immune response within the body. For these to work, boosters known as adjuvants usually need to be added. The same applies to what are known as polysaccharide vaccines, which use polysaccharides taken from the shell of a pathogen to prompt an immune response. In order to amplify the effect, polysaccharides are often bound to proteins, in which case they are referred to as conjugate vaccines.

Fermenters are used to make conventional vaccines.

Taking samples from a fermenter: with a capacity of 1,500 liters, this is the site’s largest bioreactor.
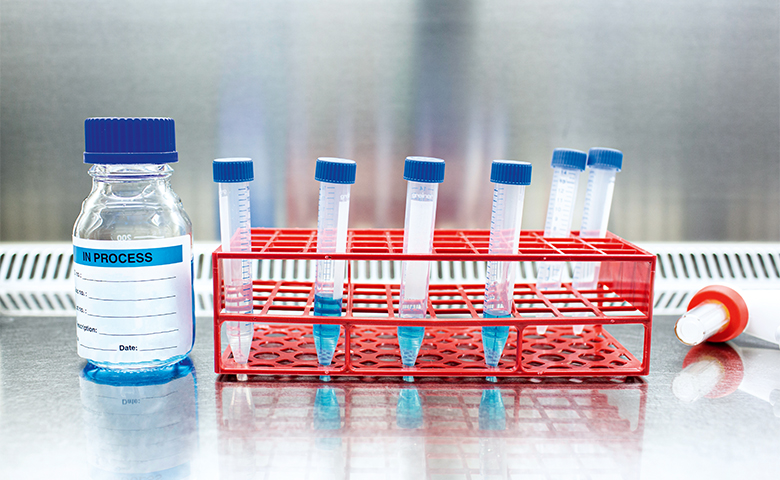
Regular quality control: vaccine samples undergoing analysis.

A New Class of Vaccines
Gene-based vaccines offer a new approach. In this case, immunization does not involve injecting pathogens or parts of pathogens – patients instead merely receive the genetic information needed to produce an individual antigen. The vaccines come in three categories: mRNA, DNA and vector vaccines.
The concept behind mRNA vaccines revolves entirely around messenger ribonucleic acid, a key molecule in the human body. As a messenger, its role is to transport assembly instructions between our genetic material and the protein factories in our cells. By synthesizing mRNA and transporting it into cells, scientists could instruct the body to manufacture a specific protein that would trigger an immune response. In the example of CureVac’s vaccine CVnCoV, the mRNA is encoded for the spike protein of the SARS-CoV-2 virus. A key issue: when an mRNA vaccine is injected into a patient, the mRNA does not enter the cell nucleus. What is more, single-stranded RNA is not compatible with double-stranded DNA. In other words, the vaccine cannot alter our genetic material. Scientists confirm this, including those from the Paul-Ehrlich-Institut, which is responsible for approving vaccines in Germany.
How mRNA Vaccines Differ from Conventional Ones
Conventional vaccine
Antigens (parts of the pathogen) are produced industrially, for example in bioreactors.
The vaccine contains the antigen.
The antigen is injected. The immune system produces antibodies that protect the body for the next encounter with the pathogen.
mRNA vaccine
The mRNA is generated by enzymes and a DNA template.
The vaccine contains only the blueprint for an antigen.
The mRNA enters the cell, where it provides instructions for producing the antigen and stimulates the immune system. Again, protection is typically conferred by antibodies.
Vaccine Production: A Science unto Itself
The processes for manufacturing different classes of vaccines are as diverse as the vaccines themselves. “Vaccine production is a science unto itself,” says Verhaagh. “Every vaccine is different, and every production process is unique, involving a considerable degree of scientific and technical expertise.” Production proceeds in multiple steps, which vary depending on the type of vaccine. In the first step, precultures of the vaccine candidate provided by the customer are prepared on a small scale. For a conventional vaccine, this is followed by scaling up production in stainless-steel tanks called fermenters or in single-use reactors. Here, bacteria multiply and produce the target active substance – in the case of a conjugate vaccine, they build the desired polysaccharides. In the next stage, the polysaccharides undergo multiple purification steps, after which they are chemically activated and lyophilized (i.e. freeze-dried) and, in the final step, bound to the carrier protein to form the finished conjugate vaccine. It’s a long, drawn-out process.
By comparison, production of an mRNA-based vaccine is more efficient. “You don’t have to culture the pathogen itself. And that eliminates a very time-consuming step,” Verhaagh explains. The starting material for production is plasmid DNA with parts of the pathogen DNA. It is transcribed by enzymes into mRNA. The active substance is then purified using chromatography. “You can’t have any kind of impurities in the production process,” she adds. Vaccine production is therefore subject to very strict hygiene regulations.
From Clinical Trials to Supplying the Market
Multiple fermenters with capacities of up to 1,500 liters are available for producing biopharmaceutical therapeutic agents and conventional vaccines in Amsterdam and at Jena and Halle, the two Biotech sites in Germany. This allows the company to adapt production volumes as needed – small quantities for clinical trials, larger amounts for supplying the market later on – all depending on the phase of development that the customer’s vaccine has reached. These facilities are about to be complemented by a new production line for mRNA-based vaccines, which will soon go on stream in Amsterdam.

Vaccines made at the Amsterdam site can be dispensed into vials if required.
Ultrapure Production Conditions
Cleanroom conditions apply to the entire production process, and spaces where finished vaccines are dispensed are subject to the most stringent cleanroom category. After production in Amsterdam, the different vaccines can either be freeze-dried or dispensed into vials. “The general rule of thumb is: the closer you get to the end product, the stricter the regulations,” says Verhaagh. For employees, this means protective clothing from head to toe. Even one grain of dust is one too many.
Several vaccine projects are currently underway in Amsterdam: while Verhaagh and her colleagues prepare for the CVnCoV production launch, the company is producing a conventional conjugate vaccine in parallel. This vaccine will soon be approved, too – though not for use against SARS-CoV-2. If CVnCoV is successfully approved, production will be expanded to include the manufacture of the mRNA drug substance. The huge number of vaccine doses needed cannot be produced any other way. For Sandra Verhaagh, that means conducting a lot of interviews these days. Whether in production, quality control or quality assurance, Wacker Biotech needs additional personnel at its Amsterdam site – in order to finally complete the vaccine puzzle.
Cornerstones of Modern Medicine
They’re on your skin, in your digestive tract, in the air and on the sea floor: we’re surrounded by billions of bacteria and viruses. Invisible to the naked eye, most of these tiny organisms are harmless, and some of them are even critical to our survival. Some, however, make us sick, potentially triggering severe, even life-threatening illnesses. Vaccines offer long-lasting protection from an array of infectious diseases, tricking the body into believing it has been infected with a pathogen. The immune system responds by producing antibodies to fight the pathogen. If an individual is then infected at some later point in time, their immune system will remember the pathogen and reactivate. This is how the vaccines work that protect us from polio, typhoid fever, cholera, hepatitis A and B, HPV and smallpox, which has been eradicated since 1980 thanks to a global immunization campaign. The list is long. And it brings home one important lesson: alongside the development of antibiotics, vaccines are the cornerstones of modern medicine. The World Health Organization estimates that vaccines save two to three million lives each year and prevent countless people from falling ill.